
Breast Cancer Foundation NZ
News & updates
Our latest news, press releases, blog posts, Pink Ribbon Bulletins & Pink Ribbon Press.
Press release
02 April 2024
Life-saving treatment for triple negative breast cancer a step closer to being funded
Pharmac has recommended Keytruda should be publicly funded for both early and advanced triple negative breast cancer.
Blog

26 March 2024
Ali's new normal
For Ali Coomber, living well after breast cancer looks like reading lots of books, regular yoga, connecting with family, and coming to terms with thoughts of recurrence.
Blog

26 March 2024
All in the same boat
Busting With Life team member Donna says, the 22 women would likely never have met, were it not for their common thread – a diagnosis of breast cancer.
Press release

15 February 2024
Exciting news: The work has started on free screening for 70-74
Today, we are celebrating a big win to ensure more breast cancer is detected early – the work has finally started on our eight year long campaign to extend free breast screening for Kiwi women aged 70-74.
Press release

14 February 2024
New drug is good news but Pharmac refuses to reconsider eligibility
Pharmac will fund ribociclib for Kiwis with hormone-positive advanced breast cancer, but the drug-buying agency has refused our recommendation to allow patients to switch drugs if they have severe side-effects.
Blog

02 February 2024
Our message this World Cancer Day: "Know your normal"
“Know your normal” is one of the key messages we share here at Breast Cancer Foundation NZ, and this World Cancer Day (4 February) we want to remind Kiwis why this is so important.
Blog

20 December 2023
Promising international trial could add more treatment options for triple negative breast cancer
Results from the international clinical trial Neo-N may increase the number of treatment options available for people with early-stage triple negative breast cancer
Pink Ribbon Bulletins

November 2023
Wow, what an October! It was so incredible to connect and share with you all - thank you for a wonderful Breast Cancer Awareness Month!
Press release

16 October 2023
New Pink Campervan kicks off inaugural tour, taking breast cancer awareness to the regions
Our new, state-of-the-art Pink Campervan has embarked on its inaugural tour, taking life-saving breast health education to all regions of Aotearoa New Zealand.
Press release

02 October 2023
What Google searches are telling us about the state of breast cancer in NZ
A dramatic surge in Google searches related to breast cancer in the last year has not correlated with an increase in mammogram participation. We're worried this may signal a concerning trend about the state of breast cancer in Aotearoa.
Pink Ribbon Bulletins

October 2023
It's Breast Cancer Awareness Month. Read the October edition of the Bulletin to know why starting conversations about breast health is so important.
Press release

28 September 2023
New Zealand shines pink for Breast Cancer Awareness Month
More than 60 iconic sites across Aotearoa New Zealand will be glowing in pink this October to show support for Breast Cancer Awareness Month.
Press release

27 September 2023
Will the next Government do enough for breast cancer?
Ahead of the election, Breast Cancer Foundation NZ has laid down a challenge to political parties to tackle breast cancer – the leading killer of New Zealand women under 65.
Pink Ribbon Press

Pink Ribbon Press - Spring 2023
PDF format - 1.9mb
Pink Ribbon Bulletins
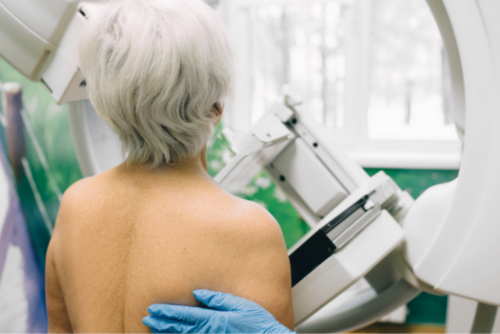
September 2023
In this issue of the Bulletin, we share how free mammograms for women aged 70-74 are another step closer to reality as well as a new patient campaign #MyLifeMatters and how you can get involved this Breast Cancer Awareness Month
Press release

31 August 2023
Free mammograms for older women receives cross-party support in Parliament
We're welcoming the cross-party support received for Dr Shane Reti's bill to increase the breast screening age.
Press release

23 August 2023
Pharmac breast cancer drug restriction denies patients “another chance at more time”
Pharmac has missed a golden opportunity to allow more Kiwis access to a new breast cancer drug, a move that would have brought New Zealand into line with the rest of the world and removed a disparity that hits Māori and Pasifika hardest.
Pink Ribbon Bulletins

August 2023
In this issue of the Bulletin, we share recent wins, how together we can make our voices heard to improve drug funding and how you can get involved in Pink Ribbon Walk for 2023
Press release

27 July 2023
Breast cancer screening bill pulled from ballot
Today Dr Shane Reti's private member's bill to increase the breast screening age to 74 has been drawn from the ballot box, taking us one step closer to our older women being able to access free mammograms.
Pink Ribbon Bulletins

July 2023
Mānawatia a Matariki! This issue of the Bulletin wishes you a happy Māori new year, welcomes the release of the Government's new Women's Health Strategy and has the details for our upcoming webinar. Read more and catch up on our news for July!
Pink Ribbon Bulletins

June 2023
The June edition of the Bulletin is dedicated to our patron Dame Rosie Horton, who passed away in May. We share some of Dame Rosie's legacy, a founding trustee and chair of Breast Cancer Foundation NZ and known as a leading philanthropist across the country
Press release
08 June 2023
Pharmac breast cancer cost-saving proposal welcome but ignores patients facing “dead-end”
We're welcoming Pharmac's proposal to replace Herceptin with a cheaper and safe alternative for HER2-positive breast cancer, but we're disappointed Pharmac's medical advisors won't widen access to this drug for certain patients who have run out of options.
Blog

05 June 2023
Suzie's reconstruction diary part 5: Feeling stronger
This is the final part of Suzie’s journal. She talks about her recovery and feeling stronger, attending her daughter's wedding, getting Covid-19 as well as her feelings about her new breasts.
Press release
01 June 2023
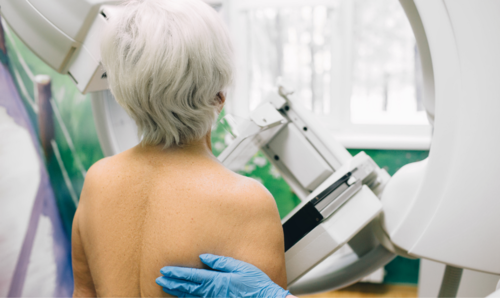
Government stalling on breast screening costs the life of one woman every month
One woman a month will needlessly lose her life to breast cancer thanks to the Government’s latest refusal to uphold its promise of lifting the breast screening age to 74.